Bullous Lung Disease or Bullous Emphysema? A Detailed Overview
When it comes to lung diseases and respiratory disorders, there are many possible diagnoses for patients. And even beyond an initial diagnosis such as emphysema, there can be an even more specific diagnosis, such as bullous emphysema.
Navigating the various types of lung diseases and respiratory disorders can therefore be overwhelming. Before you grow concerned that you may have a specific disease, the most important step you should take is to consult your physician for the appropriate tests and diagnosis. After all, there is a pretty significant difference between indigestion and a heart attack, but the two can often be confused initially.
Your physician will be your best resource to help you determine the root cause of the lung symptoms you may be experiencing. This overview will give you an idea of what to expect with bullous lung disease or a bullous emphysema diagnosis, including signs and symptoms, treatment, and outlook.
WHAT IS BULLOUS LUNG DISEASE?
When bullae develop within the lungs, that means we have a permanent, air-filled space located in the lung parenchyma or its functioning tissue. A bulla will be one centimeter or more in size and is distinguished by a thin wall.
On the other hand, a cavity in the lung has a thick wall inside of a mass or a nodule. And a pneumatocele will be a temporary space or “air tent,” often appearing after blunt trauma.
Usually, bullae in the lungs are associated with emphysema and COPD but can sometimes be found in normal lung tissue as well. The bullae will grow over time, and if they cause unmanageable symptoms may need to be removed surgically. This procedure is called a bullectomy.
HOW BULLOUS LUNG DISEASE IS CLASSIFIED
When doctors look at the surrounding parenchyma (or lung tissue), they will classify bullous lung disease into several categories.
Bullous Emphysema
Airflow obstruction is an indicator of bullous emphysema, and this occurs when the bullae form within emphysematous lung tissue. This is the most common cause of bullae formation.
Bullous Lung Disease in Healthy Lungs
A rare occurrence is when bullae form in otherwise healthy lungs, but it is possible and most likely linked to an anatomic defect. A patient in this category may have a completely normal pulmonary function.
Bullae Formation with Other Diseases
Bullae can also form in the lungs in late-stage pulmonary fibrosis. This can be seen in patients with sarcoidosis or pneumoconiosis.
Vanishing Lung Syndrome
This rare syndrome occurs typically affects the upper lobes and usually requires a surgical bullectomy.
WHO IS AT RISK FOR BULLOUS LUNG DISEASE?
Bullous lung disease risk is closely linked to prolonged cigarette smoking; however, it should be noted that exposure to other forms of smoke can contribute to the development of bullae, too.
Exposure to biomass fuels used to heat spaces and cook food can also contribute to bullous lung disease. Poorly ventilated stoves and open fires are linked to this condition, where individuals are exposed to wood, coal, peat, and kerosene.
In addition to environmental causes, bullous lung disease can also be linked to genetic factors. Alpha-1 antitrypsin deficiency, inherited connective tissue disorders, and other genetic diseases, including Neurofibromatosis 1 are possible culprits for bullae formation in the lungs.

Finally, there is also a connection between the human immunodeficiency virus (HIV) and bullous emphysema. There appears to be a tendency among HIV-positive patients who are also smokers to develop emphysematous bullae in the lungs.
SYMPTOMS: HOW DO I KNOW IF I HAVE BULLOUS DISEASE OR BULLOUS EMPHYSEMA?
Your doctor will have the best tools and resources to diagnose your condition, but some common symptoms with bullous disease may indicate you may have developed bullae in the lungs.
These symptoms include:
- Shortness of breath and difficulty breathing
- Chest pain
- Fatigue
- Loss of Appetite
- Nausea
- Nail Changes
HOW IS BULLOUS LUNG DISEASE TREATED?
Patients diagnosed with bullous lung disease will be advised by their physicians on its possible complications and airflow obstruction. Therefore, it is important upon receiving this diagnosis to follow all of your physician’s specific guidelines and always contact your medical provider immediately with any concerns, complications, or new symptoms.
Bullous lung disease treatment is similar to that of COPD, with a physician recommending:
- A smoking cessation program
- Bronchodilators, inhaled corticosteroids, and other medications to ease airflow obstruction
- When needed, supplemental oxygen
- Vaccinations for infections (such as flu and pneumonia)
- Pulmonary rehabilitation programs
In more severe cases where these treatments do not work effectively, the patient may require a lung transplant or a lung volume reduction surgery.
Another lung volume reduction option uses endobronchial valves to treat symptomatic giant bullae; this is a newer form of treatment that may work well for patients who are not suitable candidates for this surgical treatment.
Where there is an isolated bulla, a bullectomy can be performed. This procedure involves either ablation or surgical resection of the bullae. When these surgeries are successful, they can help patients with greater lung function and restore some ability to exercise.
The results of a bullectomy will vary based on a number of factors, including the size of the bulla, the condition of the patient’s lung tissue, a collapsed lung, and the level of obstruction.
As with any surgery, there are always risks, and before undergoing a bullectomy, the patient should be made aware of these risks. A patient will need to demonstrate that she has successfully completed a smoking cessation program in most cases.
The most common complication after the surgery will be a prolonged air leak that must be treated with chest tube drainage. This is a greater risk for those with emphysema in the lung surrounding the bulla. Other possible complications from the procedure include atrial fibrillation and pneumonia.
If a patient has small, poorly defined bullae, he may not be a candidate for a bullectomy. In those cases, a better treatment option may be a lung volume reduction procedure.
BULLOUS LUNG DISEASE PROGNOSIS
The progression of bullous lung disease can vary widely from patient to patient, but if left untreated, it is a near certainty the bullae will increase in both extent and size. This will lead to further air obstruction and complications in patients.
The most important first line of defense when it comes to managing bullous lung disease is a smoking cessation program. This, perhaps more than any other measure, can slow the progression of the disease.
For those patients who experience symptoms related to the bullae in their lungs (such as shortness of breath), medical treatments can provide significant relief and improvements. Inhaled corticosteroids, supplemental oxygen, pulmonary rehabilitation, and bronchodilators can all stabilize the patient’s lung function.
When a bullectomy is successful, this also contributes to greater lung function and an improved ability to exercise.
OTHER LUNG DISEASES WITH SIMILAR SYMPTOMS
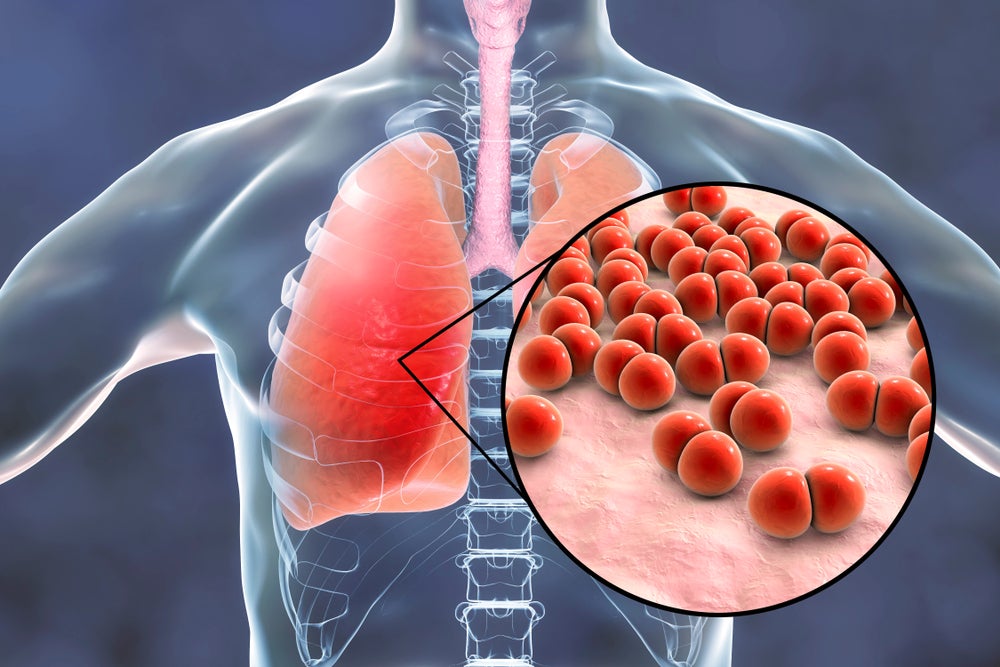
Medical diagnoses are incredibly important when it comes to lung disease, as there is a great deal of overlap between bullous lung disease and some other conditions.
A whole host of other diseases can also cause air-filled spaces or air sacs in the lung tissue, including:
- Blebs (these are basically “blisters” in the visceral pleura)
- Cystic lung disease
- Langerhans cell histiocytosis
- Lymphangioleiomyomatosis
- Tuberous sclerosis
- Lymphotic interstitial pneumonitis
- Birt-Hogg-Dube syndrome
- Pneumocystis-jiroveci pneumonia
- Cystic bronchiectasis
- Cavitary lung disease
- Cavitary malignancy
- Lung abscess
- Septic pulmonary emboli
- Rheumatoid lung nodules
- Sarcoidosis
- Progressive massive fibrosis
- Necrobiotic lung nodules
- Pneumatocele
- Pneumothorax and spontaneous pneumothorax
- Pulmonary emphysema
- Chronic obstructive pulmonary disease
As you can see, an expert diagnosis is needed to differentiate bullous lung disease from many other possibilities or another underlying lung condition, and ensure the patient receives the right form of treatment to improve lung function.
SMOKING CESSATION AND BULLOUS LUNG DISEASE
Since nothing—absolutely nothing—does more to help a patient with bullous lung disease than to successfully stop smoking, this will be a mantra repeated by physicians ad nauseum. As mentioned above, a bullectomy will not be performed on a patient without successfully completing a smoking cessation program.
Fortunately, physicians can recommend a wide range of programs available to help in this regard, bearing in mind that many patients find it difficult (if not impossible) to quit “cold turkey.”
Your doctor may suggest:
- Support groups for smoking cessation
- Medications to control nicotine cravings
- Hypnosis
- Meditation
One of the best things you can do is reach out to family, friends, co-workers, and neighbors for help when you decide to quit smoking. Creating a network of support and a group that will hold you accountable will go a long way toward helping you achieve your goal of quitting smoking.
Some patients work well by creating a sort of “reward” system. For example, you might promise yourself at the six-month mark, you will splurge on an exercise bike; at the one-year mark, you might treat yourself to a beach vacation. Paying for these items may be easier than you think once you stop paying for cigarettes!
Average Lung AirPhysio
ENJOY BETTER BREATHING - Use this 100% Drug Free Device - AIRPHYSIO
Recent Posts
Sports AirPhysio
IMPROVE YOUR SPORTING PERFORMANCE - Use this 100% Drug Free Device - AIRPHYSIO

AirPhysio Child
BETTER BREATHING FOR YOUR CHILD - Use this 100% Drug Free Device - AIRPHYSIO

Categories
- asthma (2)
- atelectasis (2)
- bronchiectasis (2)
- copd (3)
- cystic-fibrosis (45)
- featured (10)
- uncategorized (2)

