THE ULTIMATE GUIDE TO LUNG HEALTH
By Life Wellness Healthcare & The Portable Airphyisio Lung Cleaning Device
THE SYMPTOMS OF LUNG DISEASE
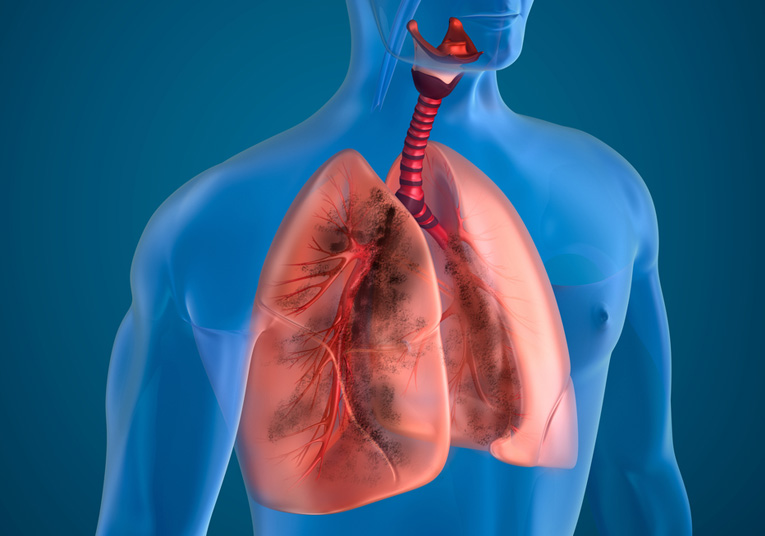
Lung disease may manifest in various ways, each with its own symptoms. Some common symptoms of lung disease include coughing, wheezing, chest pain, and shortness of breath.
Breathing Difficulties

Breathing difficulties can signify many lung diseases, including bronchitis, emphysema, and pneumonia. A tight chest, difficulty catching your breath, and feeling like you can’t get enough air are signs that something may be wrong with your lungs.
Breathing difficulties are often caused by inflammation in the airways or lungs. This can make it hard for air to move in and out of your lungs, leading to shortness of breath.
A buildup of fluid in the chest, in some situations, can cause difficulty breathing. This is called pulmonary edema and can be a sign of heart failure.
Shortness of Breath

Shortness of breath can be noticeable both when active and at rest. If you have shortness of breath, it may become difficult to do everyday activities such as walking upstairs or carrying groceries.
You may notice shortness of breath when your lungs can’t get enough oxygen or when they’re not getting rid of carbon dioxide.
Shortness of breath can cause panic attacks in some people, worsening shortness of breath.
Coughing

Coughing is one of the most prevalent symptoms of lung diseases like bronchitis, chronic obstructive pulmonary disease (COPD), and pneumonia. A cough might also be a symptom of other respiratory illnesses, such as the common cold or flu.
Coughing can be intense and persistent, or it may come and go. It can be either dry or wet, depending on the source of the cough. Coughing can last for days, even weeks at a time.
Wheezing

Wheezing is a shrill, high-pitched whistle produced when you breathe. It can be caused by several different lung diseases, including asthma, bronchitis, COPD, and pneumonia.
Wheezing can also be caused by heart disease, obesity, and even anxiety. Wheezing can be heard when talking, laughing, or even coughing.
Decreased Exercise Ability

People who exercise regularly may notice that their ability to do so has decreased. This can be a sign of lung disease, especially if the shortness of breath is noticeable during exercise.
The difference can be only small, but it can add up and make it difficult to do the things you love over time. You may feel out of breath sooner than usual when doing a cardiovascular activity.
A Persistent Cough That Won’t Go Away

Sometimes coughs can last months and never seem to go away. This is called a chronic cough, which can be a sign of lung diseases such as COPD or bronchitis.
People often ignore persistent coughs, thinking they’re just a cold or flu that will eventually disappear. However, if you have a cough that lasts more than a few weeks, it’s essential to see a doctor to rule out underlying lung diseases.
Regurgitation of Blood or Mucus

Regurgitation of blood or mucus can be a sign that something is wrong with your lungs. This may occur when you cough, spit or even clear your throat.
Mucus can cause chest congestion, making breathing difficult. If you see blood in your mucus, it’s important to see a doctor right away, as this can be a sign of a more severe lung condition.
When you are sick, it is important to check your mucus. It can give you a good idea of how your lungs are doing. If it is white and clear, then your lungs are healthy. If it is yellow or green, your lungs may be infected.
Chest Pain

A tight chest, or chest discomfort, might be a symptom of lung problems, especially if it is accompanied by shortness of breath or coughing. This sort of chest discomfort is frequently the result of an inflammation in the lungs or airways.
If you or someone you know has one of these problems, go to a doctor as soon as possible. Many individuals ignore minor indications and symptoms of lung illness, resulting in more significant health problems down the road. If you have any concerns about your lungs, do not take a chance on your health.
DIFFERENT TYPES OF LUNG DISEASES
Several lung disorders might impact your breathing, each with its own symptoms. Lung diseases can be life-changing, and some can even be fatal. The following are some of the most prevalent lung conditions:
Bronchitis
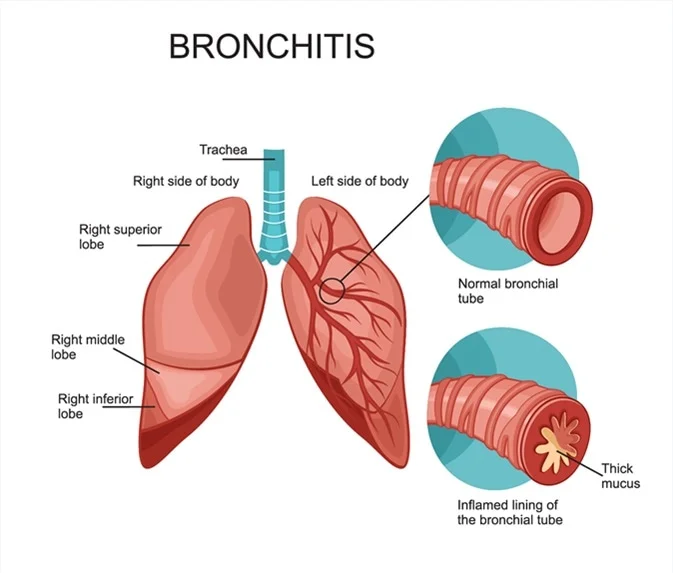
Bronchitis is a type of lung inflammation characterized by inflamed bronchi. Coughing, chest discomfort, shortness of breath, and wheezing are bronchitis symptoms.
At the top of your windpipe (trachea), the two main airways branch off to either side. These tiny, narrow passageways in our lungs are known as bronchiole. The walls in these passageways produce mucus that traps dust or other irritants that could otherwise cause inflammation if this protective layer did not filter them out; most cases happen when an infection irritates them, causing their production level to exceed normal for someone’s health status.
Bronchitis and emphysema are prevalent in individuals with COPD. Chronic cough, shortness of breath, and wheezing are signs of COPD.
Chronic bronchitis is an infection that can last for months or years. A common cause of breathing problems is chronic bronchitis, which can have serious consequences if not treated. It’s either acute or chronic, and it affects the airways of your throat in different ways depending on how long you have had this disease. For example:
- Acute bronchitis lasts up to three weeks with symptoms like coughing fits accompanied by mucous production; these tend to happen once but may come back again after prolonged periods without treatment.
- Chronic bronchitis is a more serious long-term condition that can last up to several months (or even years), With symptoms like a daily cough that produces mucus and difficulty breathing.
Emphysema
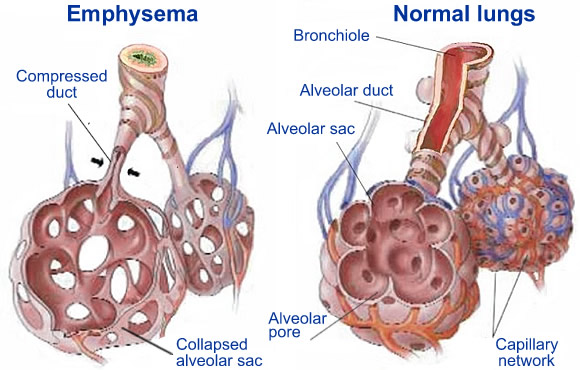
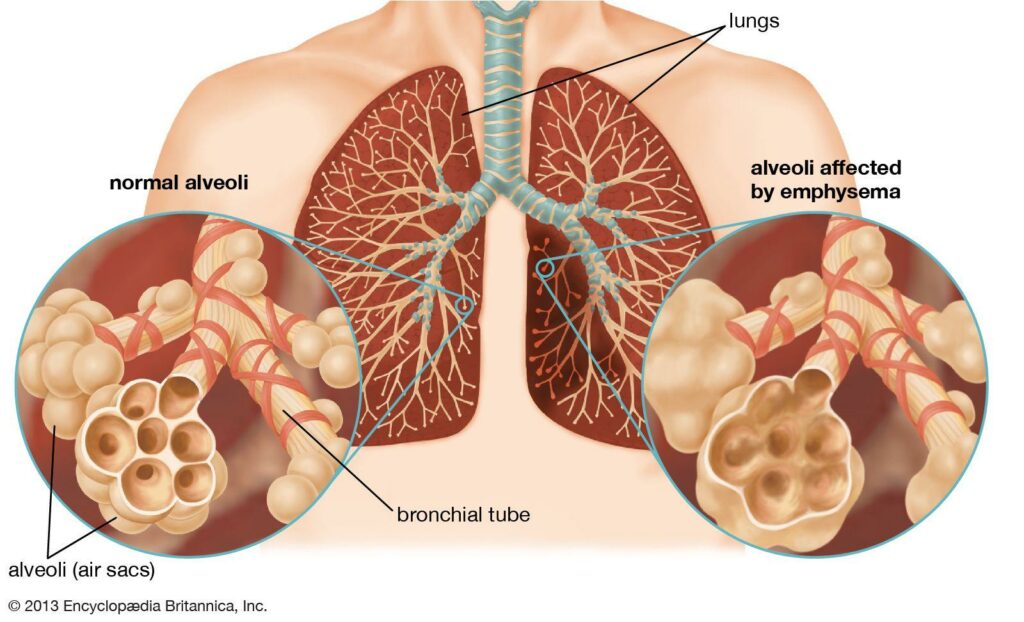
Emphysema is an illness that causes you to have shortness of breath. In people with an empty state, the air sacs in their lungs (alveoli) are damaged over time, leading to larger spaces for oxygen instead of small ones because it damages inner walls, making them unable or less able to retain carbon dioxide appropriately.
As a result, less oxygen is absorbed into the circulation, and carbon dioxide builds up, causing breathlessness.
Emphysema occurs mainly in smokers but can also occur in people exposed to secondhand smoke, air pollution, or dust. People aged 40 or older are at increased risk of emphysema. This is due to built-up damage over time.
Treatments are frequently designed to reduce symptoms and increase the quality of life. Emphysema cannot be cured, but quitting smoking is the most effective strategy to keep it from progressing.
Lung Cancer
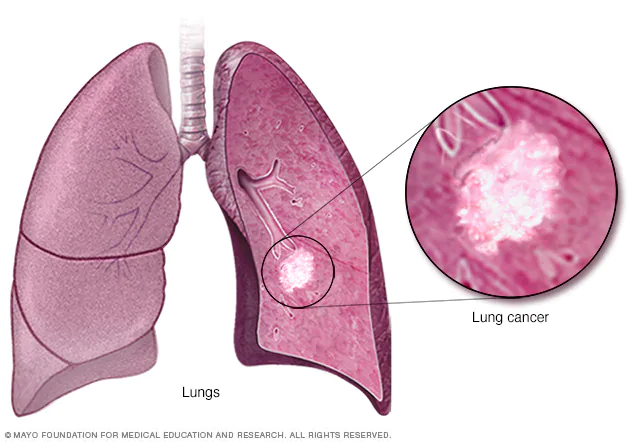
The most common form of cancer death in both men and women is lung cancer. Cough, chest discomfort, shortness of breath, and weight loss are signs of lung cancer.
Cancer of the lungs is an acute condition in which uncontrolled cells develop in the lungs. These can invade nearby tissues and form tumors, which may spread throughout your body via metastasis or “spreading” to lymph nodes or other parts of your system, such as bone marrow skin itself.
Most lung cancer cases are caused by smoking, but exposure to secondhand smoke, air pollution, or asbestos can also increase your risk of developing the disease.
Lung cancer is the most common type of cancer in men and women over the age of 55, although it can affect anybody at any age.
COPD
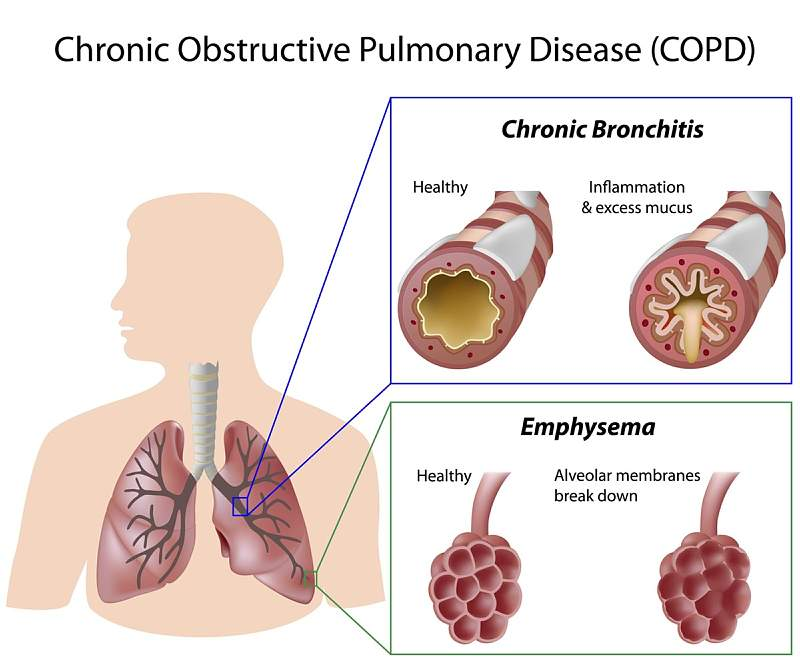
COPD stands for chronic obstructive pulmonary disease, which is a group of conditions that result in airway obstruction and respiratory-related issues.
It includes emphysema and chronic bronchitis, making it difficult to breathe by stopping airflow in your lungs. You may need to use an inhaler before going anywhere, even if it’s just one flight of stairs.
People who have chronic obstructive pulmonary disease (COPD) have been breathing in dangerous particles, such as cigarette smoke, dust, and gases, for an extended period. People with COPD are more likely to get lung cancer, heart disease, and other respiratory issues than those without the condition.
COPD is most common in people who are elderly, smokers, or those who have been exposed to secondhand smoke.
Pneumonia
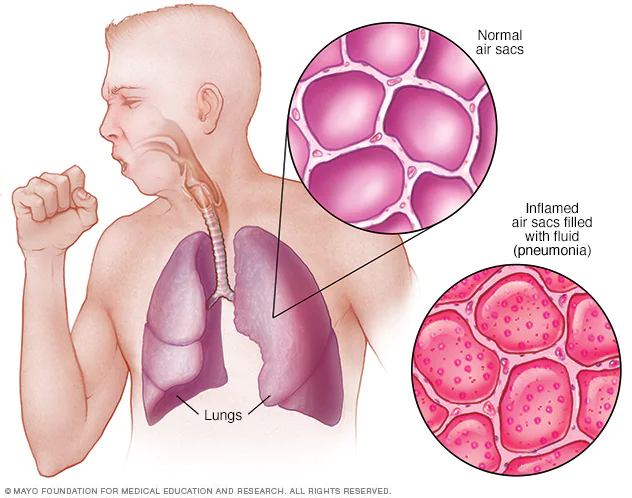
Pneumonia is an inflammatory condition of the lungs’ air sacs that causes inflammation. The inflammation can cause cough with phlegm and pus, fever, chills, and difficulty breathing; many organisms contaminants could be responsible for this condition, including bacteria, viruses, and fungi.
Pneumonia is a severe illness that requires treatment with antibiotics. Pneumonia starts with a cold or the flu, which can lead to an infection in the lungs.
Chest discomfort, shortness of breath, fast breathing, mucus coughing up, and a feverish or shivering feeling are signs of pneumonia. It can be deadly if not treated promptly. It is common to develop pneumonia in damp and cold climates.
Pulmonary Edema
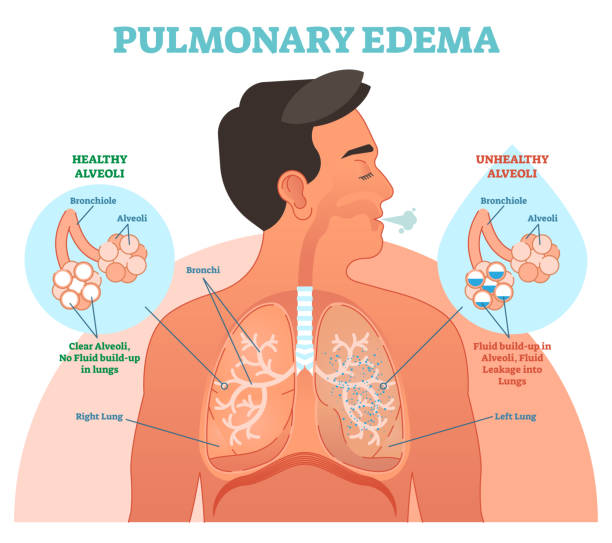
Pulmonary edema occurs when there is an overabundance of liquid in the lungs. The air sacs are filled with this liquid, making it difficult for you to breathe correctly, and it can lead to many other complications if left untreated!
Symptoms of pulmonary edema include shortness of breath, difficulty breathing, coughing up mucus, rapid heart rate, and confusion or disorientation.
Pulmonary edema can be caused by many things, including heart failure, pneumonia, smoke inhalation, drug or alcohol abuse, and extreme strenuous activity. The most common age of occurrence is 65 years old.
Pulmonary edema has a high fatality rate if not treated immediately. However, with proper medical care and treatment, the prognosis is good.
Treatment for pulmonary edema includes oxygen therapy, diuretics, and nitroglycerin. In severe cases, a heart-lung machine may be necessary.
Tuberculosis
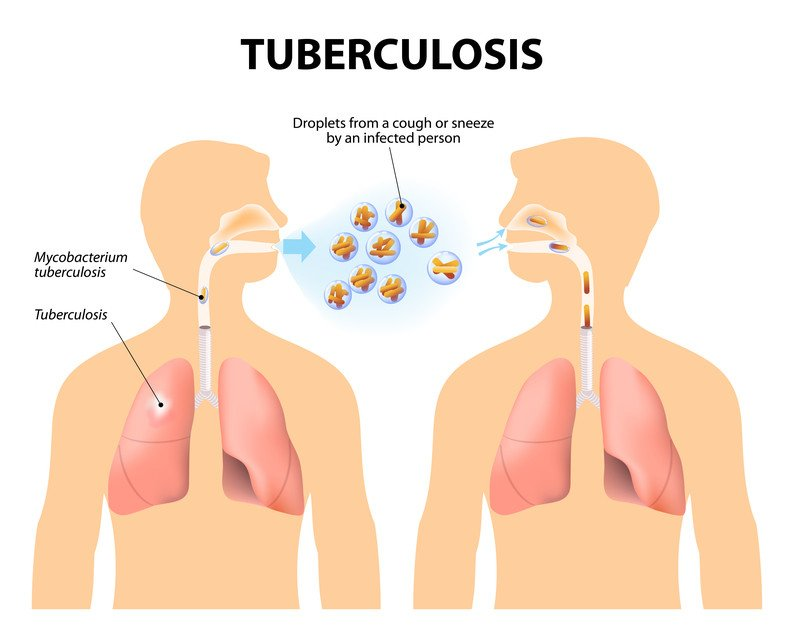
Tuberculosis, or TB, is an incurable lung disease caused by the Mycobacterium tuberculosis bacteria.
TB can affect any organ in the body, although it is most frequently seen in the lungs. When an infected person coughs or sneezes, the virus is transferred through the air. It’s most common in countries with a lot of poverty and uncleanliness.
Symptoms of TB infection include chest pain, fever, bleeding from the lungs, difficulty breathing, and weight loss.
TB is most commonly found in people aged 20 to 40 years old, but it can occur.TB is treated with anti-TB drugs and surgery to remove the diseased tissue. A single course of antibiotics may be sufficient to cure the condition in some situations.
People with serious underlying diseases, such as HIV/AIDS, are more likely to get TB than others.
Asthma
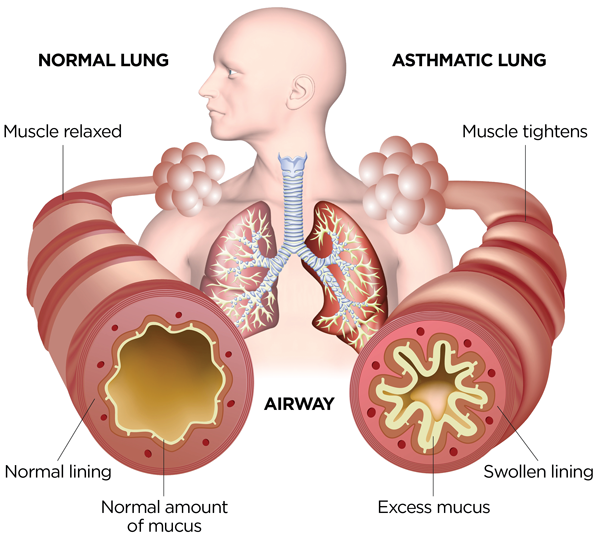
Asthma is an airway allergy that results in wheezing, chest tightness, and shortness of breath. It affects people of all ages, although it is most common in young children.
Asthma is characterized by an inflamed airway. The hypersensitivity of the airways to certain stimuli, such as allergens, smoke, or cold air, causes inflammation. When the airways are exposed to these triggers, they become narrow and constricted, making breathing difficult.
Asthma is a long-term condition that may be treated with medicine. Inhalers, nebulizers, and steroids are some medicines used to manage asthma.
If you have asthma, avoid the things that aggravate your condition and visit your doctor regularly. Asthma can be a severe condition, but it might be manageable with proper treatment.
Asthmatics can use inhalers to help them breathe when they have an asthma attack. Inhalers contain medicine that relaxes the muscles around the airways, making it easier to live. There are many different inhalers available, and your doctor can help you choose the best one for you.
Nebulizers are a type of asthma treatment often used in tandem with other medicines. Nebulizers are machines that turn the medicine into a mist, which you then breathe in. This is a good option for people who have difficulty using an inhaler.
Steroids are another type of medication used to treat asthma. Steroids help reduce inflammation in the airways and make it easier to breathe. They are usually taken in pill form but can also be given through an inhaler or nebulizer.
If you have asthma, it is critical to visit your doctor regularly. This will help keep your asthma under control and minimize the chances of having an asthma attack.
HOW IS LUNG DISEASE OR DISORDER DIAGNOSED?
There are multiple ways to diagnose different lung diseases. A medical history and a physical examination are usually the first steps a doctor takes. Following this, diagnostic tests will be ordered to confirm the diagnosis.
Lung (Pulmonary) Function Tests
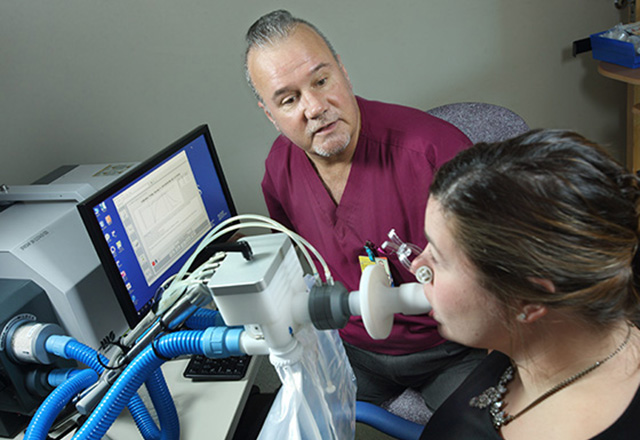
The lungs are complex organs that require the right balance of airflow and capacity to function at their best. Pulmonary function tests (PFTs), such as spirometry or volumetric, measure this vital statistic in terms you can understand-lung volume, rate(s) of flow/ ventilation, and gas exchange.
Spirometry – a method for measuring the force of airflow through your lungs. A spirometer has an elastic mouthpiece hooked up to a small electronic machine, which will record how hard you are breathing and transmit this information wirelessly so that it can be analyzed by healthcare professionals looking at charts or graphs representing thousands of hours’ worth of patient tests!
Plethysmography – a type of medical test that measures the size and function of blood volume in your body. You sit or stand inside an air-tight box, which looks like a short telephone booth with markings on all sides, so you can’t move around while getting this procedure done!
These are what are measured during a PFT test:
- Tidal Volume (VT) – This is the amount of air breathed or exhaled during normal breathing.
- Vital Capacity (VC) – The maximum amount of air that may be exhaled after taking in as much as possible.
- Functional residual capacity (FRC) – The amount of air still in one’s lungs after a normal exhale.
- Residual Volume – This is the amount of air still in the lungs after exhaling all you can.
- Total Lung Capacity – The amount of air that a person’s lungs can contain when filled to the brim with as much air as possible.
- Forced Vital Capacity (FVC) – This is the quantity of air expelled forcefully and swiftly after you’ve gotten as much air as possible.
- Peak Expiratory Flow Rate (PEFR) – This is the maximum volume of air you can exhale from your lungs.
Chest X-ray
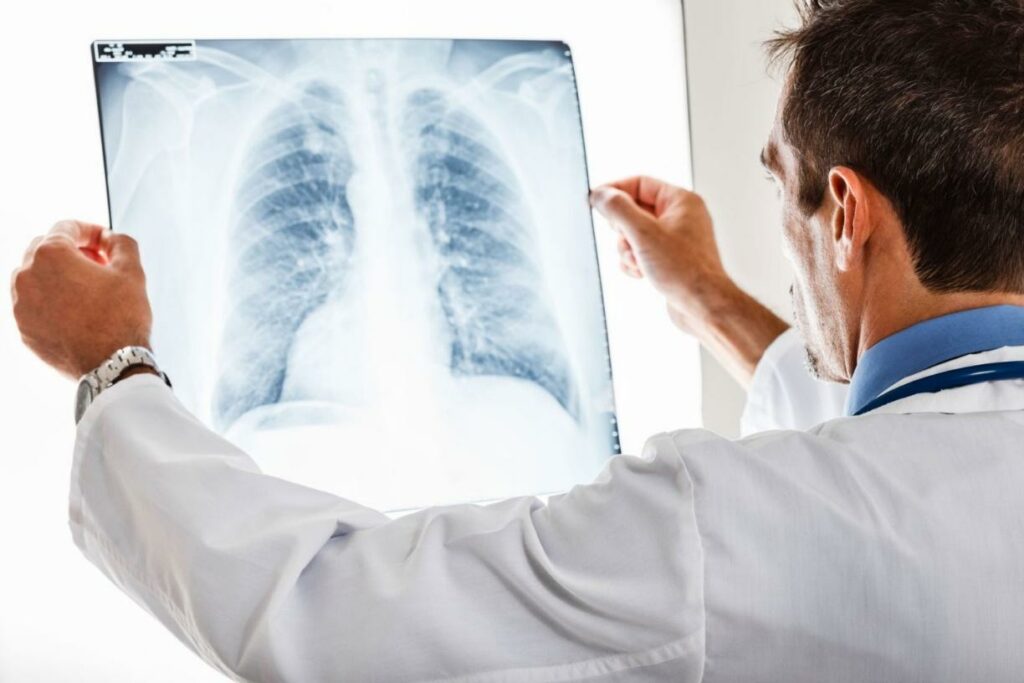
A Chest X-ray is useful in diagnosing many lung diseases, including pneumonia, lung cancer, and tuberculosis. The X-ray will show the size and shape of your lungs and any abnormal growths or masses.
High-energy waves are passed through the body to generate an X-ray image via X-ray. Different tissues absorb these waves differently so that they will appear differently on the X-ray.
X-rays are fast, painless, and relatively inexpensive. They are also non-invasive, so they don’t require any needles or injections.
The only negative side of X-rays is the radiation they give off. This radiation can potentially cause cancer, so it’s essential to minimize your exposure to X-rays as much as possible.
CT Scan
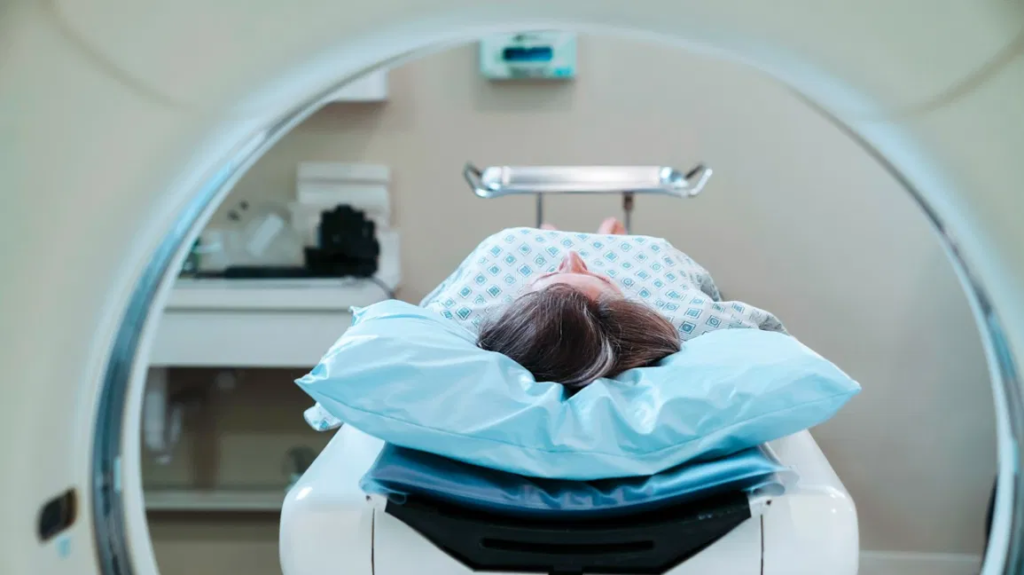
The CT or Computed Tomography scan is a type of medical imaging used in radiology to obtain detailed interior images without radiation.
CT technology has led to an increase in the diagnosis of pulmonary nodules, which are collections of abnormal tissue within the lungs. These early manifestations of cancer may not produce any physical symptoms yet. Still, this procedure can detect them before they grow into more serious health issues such as lung cancer.
A recent development with medical researchers is their ability to generate detailed images that provide insight into what type of cell growth occurs at each location throughout the body, specifically when it comes down to imagery around internal organs like your lungs!
CT scans have the advantage of being a low-dose radiation procedure that may be used to examine almost any region of the body. CT images take around 15 minutes to produce and are typical in most hospitals.
Arterial Blood Gas Analysis
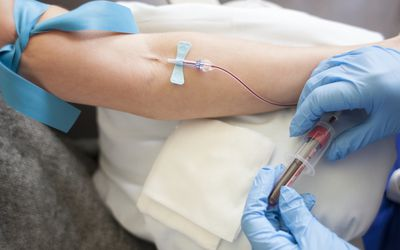
The arterial blood gas test is the most important medical test for people who have respiratory problems. It’s used to measure how well your lungs are working and what kind of gases they exchange with each breath and check on the acid-base status.
The test is conducted by obtaining a small amount of blood from an artery, usually the wrist. The blood is analyzed to determine the amount of oxygen and carbon dioxide.
Respiratory illnesses such as asthma, emphysema, and pneumonia can be diagnosed with ABG testing. They can also help determine the best treatment for these conditions.
The ABG test takes around 15 minutes to complete and is usually done in a hospital or doctor’s office.
Laboratory Tests
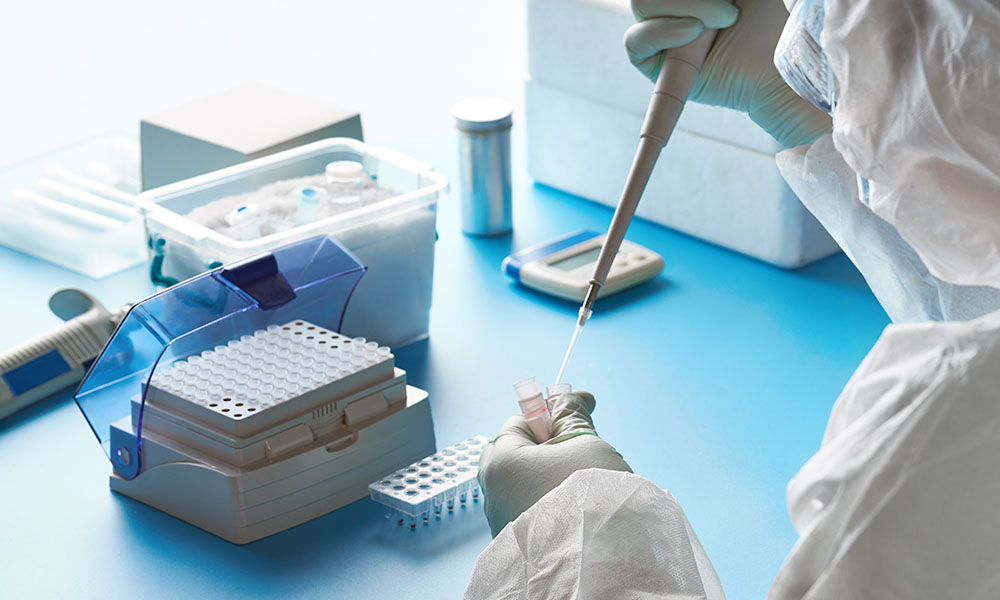
Lab tests are used to diagnose lung diseases like tuberculosis, Legionnaires’ disease, and histoplasmosis. They might also be utilized to discover the origin of a respiratory illness.
Blood culture and sputum culture are two of the most frequent tests for lung illness.
- Sputum Culture – a test that grows bacteria from a sample of mucus coughed up from the lungs.
- Blood Culture – a test that checks for bacteria in the blood.
These tests can take several days to weeks to complete. They are usually done in a hospital or doctor’s office.
WHAT CAN CAUSE LUNG HEALTH PROBLEMS?
In this modern era, multiple day-to-day life choices and environmental exposures could be the potential cause of lung health problems.
Some general causes are cigarette smoking, air pollution, exposure to radiation, asbestos, and working with hazardous materials. More specific causes can include bird droppings, chemical fumes from paint or plastics, coal dust, silica dust, and welding fumes.
The difficult thing is that some of these exposures can cause problems immediately, while others may not cause any problems for years or even decades. This is why it’s so critical to be informed about the hazards and take precautions to preserve your lungs.
Tobacco Smoke

Tobacco smoke is the leading cause of lung cancer and is also a significant risk factor for other respiratory diseases such as COPD, emphysema, and bronchitis.
Smoking is a slow killer. The earlier you stop smoking, the more likely you avoid these diseases. There is no safe level of tobacco smoke exposure. Even little doses can be harmful.
If you have asthma, cigarette smoke can trigger an attack or make it worse. The secondhand smoke emitted by smokers, pipes, and cigars is believed to cause lung cancer, heart disease, and stroke. It also raises the chance of respiratory infections in developing youngsters.
Many parents smoke around their children, which causes severe problems for children in the future with lung health. The damage from cigarette smoke can take years to build up and cause problems.
Air Pollution

Air pollution can lead to cancer and asthma in some people. There is good evidence that outdoor air causes these diseases, so it’s important for people who live or work outdoors regularly (or will be working near heavy traffic) to wear masks when outside during particularly bad weather events like storms which bring in more particles into our atmosphere.
It has been proved that if children are exposed to air pollution for an extended period, their lungs may develop differently. There’s also new evidence indicating that these patients have a higher chance of getting asthma!
Ground-level ozone smog is a mixture of VOCs and NOx that forms when sunlight breaks down volatile organic compounds in the air.
When there’s little or no wind, ozone concentrations can reach unhealthy levels. Ozone is a gas that can cause chest pain, coughing, and shortness of breath. It can also exacerbate asthma and other respiratory problems.
The second type of harmful pollution is fine particulate matter, also called soot, and found in the air mainly as a by-product of combustion such as auto or diesel exhaust. It can come from power plants too!
Pollution-caused lung health problems are becoming more common as we learn more about the long-term effects of exposure to air pollution.
Radon Gas
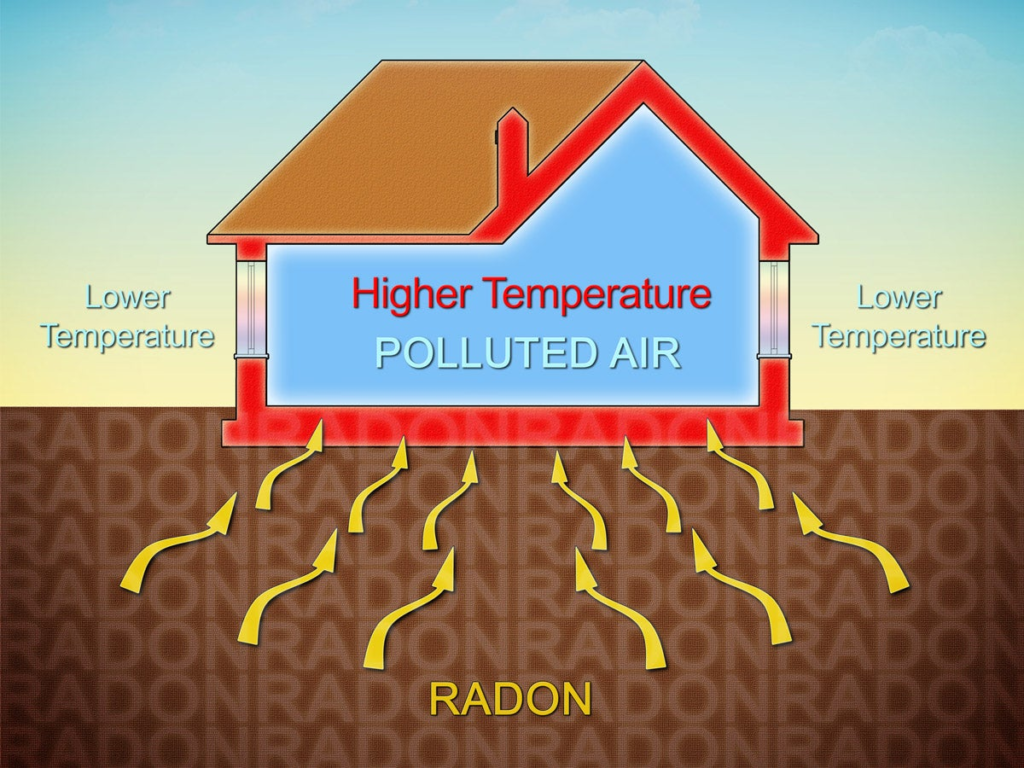
It’s important to know the risks of radon, as it is second only in frequency behind cigarette smoking. High levels can cause cancer and increase your chances of developing lung-related illnesses such as bronchitis or emphysema.
Although radon is a naturally occurring gas, people can be exposed to it by breathing in air that comes from cracks and gaps. Exposure mainly occurs when there are openings or breaks at ground level, which allow access for radiation inside an area’s crust – this includes rock formations as well!
Radon gas is a slow killer. The effects of exposure may not be felt for years, so it’s important to get your home tested.
Asbestos

Asbestosis is a lung disease that results from breathing in asbestos fibers. Prolonged exposure to these toxic particles can cause scarring and shortness of breath in the lungs, leading many people exposed years later to asbestiform fibrosis. This incurable form affects only half of your body’s cells.
The effects of long-term asbestos exposure are typically not seen until 10-40 years after initial contact. Symptoms can vary in severity and may go unnoticed if they’re relatively minor at first but will develop into more severe conditions over time unless appropriately treated with a variety of treatment options available, including surgery or medicine prescribed by your doctor.
In the 1970s, the federal government started regulating asbestos and its by-products. As a result, most people who develop asbestosis did so on the job before this regulation came into effect.
Asbestos is frequently used in older structures. If you’re not sure if your house contains asbestos, get it checked by a specialist.
Chemical Fumes and Vapor

Many chemicals can cause lung damage if inhaled, and these vary depending on the industry. Some of the most common include:
- Ammonia – found in cleaning products
- Chlorine – found in bleach and swimming pools
- Diesel exhaust fumes
- Hydrochloric acid – used in manufacturing
- Isocyanates – used in spray paints
If exposed to enough of these chemicals, they can cause significant lung damage. Coughing, wheezing, shortness of breath, and chest discomfort are among the symptoms. If you work with any of these chemicals, it’s important to wear a mask and ventilate the area properly.
COMMON THERAPIES OF LUNG DISEASE

Treating lung disease can be difficult, as there is no one-size-fits-all approach. The most important thing is to stop smoking and avoid exposure to harmful fumes and chemicals. You should also avoid triggers such as dust mites, pet dander, and pollen if you have asthma. Below are some of the most effective treatments for lung disease:
- Corticosteroids
- Bronchodilators
- Oxygen therapy
- Inhalers
If your COPD makes it difficult to breathe, you’ll most likely be prescribed an inhaler. This gadget allows you to breathe medication straight into your lungs. A doctor or nurse will instruct you on the proper use of an inhaler. COPD inhalers come in a variety of shapes and sizes. The following are the most common types:
- Short-Acting Bronchodilator Inhalers – typically used to relieve symptoms on an as-needed basis. When you’re feeling short of breath, take a short-acting inhaler up to four times each day.
- Long-Acting Bronchodilator Inhalers – long-acting bronchodilator inhaler will be suggested if you have symptoms throughout the day. These are taken once or twice a day to prevent symptoms.
- Steroid Inhalers – A GP may recommend a steroid inhaler as part of your therapy if you’re still becoming breathless after taking a long-acting inhaler or if you have frequent flare-ups (exacerbations). Corticosteroid medications, which are included in steroid inhalers, can help to decrease inflammation in your airways. In most cases, steroid inhalers are administered as part of a combination inhaler that also contains a long-acting drug.
Oxygen Therapy
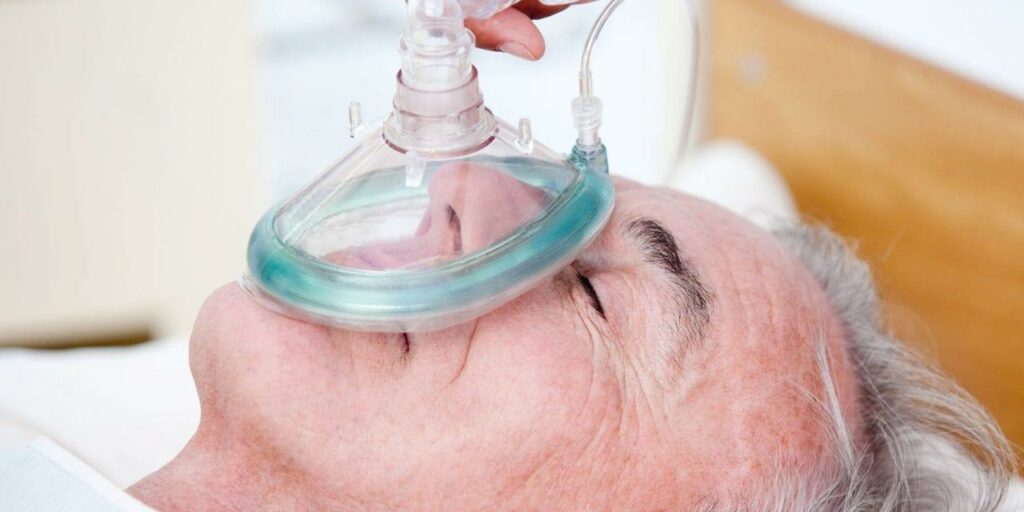
It’s a method of increasing the amount of oxygen in your lungs. Your doctor or nurse may refer to it as “supplemental oxygen.”
You can get supplementary oxygen in various ways when you start oxygen treatment, but you’ll almost certainly begin with a nasal cannula. This gadget consists of two little tubes that go into your nostrils and a longer air tube that connects to an oxygen tank. This is the most prevalent method of oxygen treatment.
In severe cases, a surgeon makes a hole in the windpipe in the most critical situations (trachea). A line extends from the oxygen tank to your windpipe, passing through a tiny hole in your neck. Transtracheal treatment is the term for this procedure.
The benefits of oxygen therapy usually last as long as you continue to use it. However, if your condition worsens and you no longer require oxygen therapy, your doctor will likely stop prescribing it.
Palliative Care

If your lung disease is advanced and little can be done to improve your health, palliative care may be recommended. This type of care is focused on making you as comfortable as possible and managing your symptoms. It’s also an excellent resource for caregivers, offering support and advice.
Palliative care usually involves a team of specialists, including a doctor, nurse, social worker, and chaplain. The team will work with you to create a personalized care plan that meets your needs.
Palliative care can be provided in various settings, including hospitals, hospices, and at home. Your doctor will work with you to create a plan that meets your needs. A typical program may contain the following:
- Walking, cycling and strength exercises are examples of physical fitness training adapted to your requirements and abilities.
- For you and your family, information about your illness is essential.
- Dietary suggestions
- Emotional and psychological assistance
Tablets
If inhalers aren’t enough to control your symptoms, a doctor may prescribe pills or capsules. Below are the different types of pills and capsules that are used to treat lung disease breathe:
Theophylline Tablets
Bronchodilators include theophylline. Although the specific mechanism of action of theophylline is unknown, it appears to decrease swelling (inflammation) in the airways and relax the muscles that border them.
Theophylline is taken twice a day in the form of pills or capsules. During therapy, you may need to undergo regular blood tests to assess the amount of medication in your blood. This will aid a doctor in determining the appropriate dose to treat your symptoms while minimizing adverse effects.
Mucolytics
A mucolytic drug called carbocisteine may be prescribed if you have a chronic chesty cough with a lot of thick phlegm.
Mucolytic medications thin the phlegm in your throat, making coughing easier. Carbocisteine is taken three or four times a day as pills or capsules. If carbocisteine does not relieve your symptoms or you cannot take it due to medical reasons, you can try acetylcysteine, a mucolytic drug.
This is a powder that has to be mixed with water. The odor of acetylcysteine powder is unpleasant, but it should go away after combining it with water.
Pharmaceutical – Homeopathic
If you are having problems with your breathing, homeopathic medicine may be prescribed in addition to your other medications.
Homeopathic medication is a form of alternative medicine that uses very small doses of remedies made from natural substances, such as plants or minerals. Homeopathic medicines are usually taken orally in the form of tablets or drops.
Some examples of homeopathic medication include:
- Arsenicum Album: for shortness of breath and a cough that gets worse at night
- Natrum Muriaticum: for difficulty breathing, a rattling sound in the chest, and coughing up greenish-yellow mucus
- Pulsatilla: for coughing and wheezing that gets worse at night
You must take it exactly as your doctor tells you when prescribed a homeopathic remedy. Don’t stop taking any of your other medications without talking to your doctor.
The great thing about homeopathic medicine is that it’s rarely associated with any side effects due to the natural ingredients.
OPEP Devices
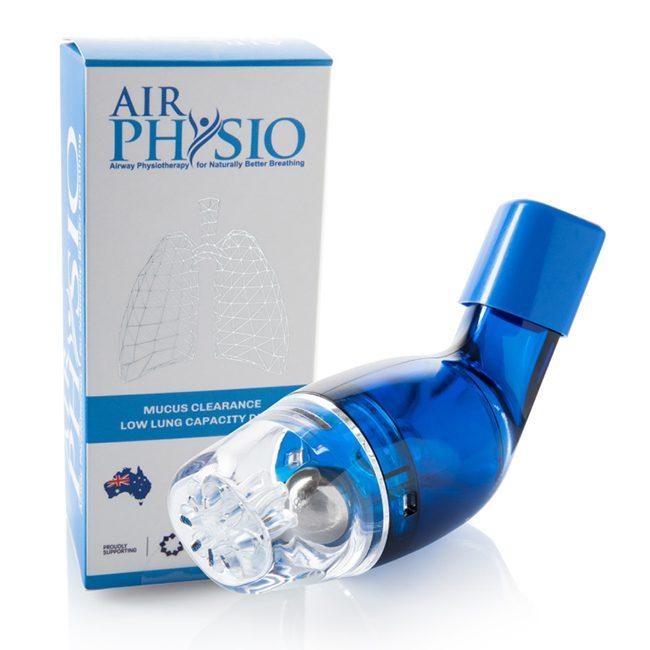
An OPEP device is a handheld device that you use to help improve your breathing. OPEP devices are used to treat shortness of breath, wheezing, and other symptoms associated with lung disease. Many different OPEP devices are available, so it’s essential to discuss which type would be best for you with your doctor.
These innovative devices can help you breathe more easily, and they are becoming increasingly popular as a treatment for lung disease. We will be discussing OPEP devices in more detail in a future blog post, so stay tuned!
BENEFITS OF TREATING LUNG DISEASE

There are many pros to treating lung disease. Treatment can help improve your quality of life, allow you to live longer, improve your sex life, give you more energy, and make you less anxious. Lung disease treatments can be very beneficial for those who suffer from the condition. If you have been diagnosed with lung disease, it is important to discuss treatment options with your doctor. Many different treatments are available, and each person’s needs will vary.
Treatments Improve your Quality of Life

Lung disease treatment has been shown to improve the overall quality of life. This is due to many of the other benefits of the treatment, such as an increase in physical function and lessened symptoms. According to research, those who begin pulmonary rehabilitation within three months of being admitted to the hospital for lung disease-related disorders have a much-reduced risk of dying after one year than those who start later or do not participate in pulmonary rehabilitation. More evidence shows that pulmonary rehabilitation improves people’s symptoms, exercise ability, and overall quality of life.
Improve Sex Life

Lung disease causes wheezing, shortness of breath, coughing, and other respiratory symptoms. These symptoms can make your sex life difficult. However, many people with lung disease can and do have fulfilling sex.
Although sex may be less frequent, sexual activity and fulfillment are still achievable. If you use oxygen therapy, you should also use it before and maybe even during sex. Your oxygen supply company may be able to provide extended tubing, so there is more space between you and your oxygen tank. This can help you with your breathing and alleviate the restriction of movement that occurs with oxygen tubing that is too short.
Sometimes people with Lung disease have bronchospasms during sex. Use your bronchodilator before intercourse to lessen this risk. Keep it on hand in case you need it during or after sex. This will also help to reduce the possibility of breathlessness.
Better Exercise

Pulmonary rehabilitation can also help you exercise. If you have trouble breathing while exercising, your doctor may recommend a pulmonary rehabilitation program. These programs mix medically supervised group exercise with disease care and education to address your particular challenges.
Rehabilitation can help you improve your lung function and symptoms, allowing you to do daily tasks with less pain and live a more active life. Exercising can be difficult when you have lung disease and have trouble breathing. Regular physical activity, on the other hand, can strengthen your respiratory muscles, increase your circulation, help you use oxygen more efficiently, and reduce your symptoms.
Physical activity has been shown in studies to help protect against lung disease onset and progression, as well as to reduce the loss of lung function. Higher amounts of activity resulted in larger advantages, according to the study.
More Energy

Tiredness and a lack of energy are common symptoms of lung disease fatigue, and they can have a significant impact on a person’s quality of life. Lung disease patients have difficulty getting oxygen into their lungs and releasing carbon dioxide. Both a lack of oxygen and a buildup of carbon dioxide can make a person feel fatigued and depleted of energy.
Treatment can assist in alleviating symptoms such as fatigue. Shortness of breath can be managed and help make it easier to breathe, which can help with fatigue. A doctor may prescribe one or more of the following drugs and lifestyle changes to assist a person in breathing more easily and manage their fatigue:
bronchodilator inhalers, which open or dilate the airways, steroid inhalers, which lessen lung inflammation and shortness of breath in patients with low oxygen levels, can be relieved with oxygen therapy. Practicing breathing exercises, eating a balanced diet, exercising regularly, staying hydrated, and having good sleeping habits
Less Anxiety

For a variety of reasons, many patients with lung disease experience anxiety. When you have difficulty breathing, your brain sounds an alert to let you know something is wrong. Anxiety or panic may result as a result of this.
Inquire with your doctor about being referred to a pulmonary rehabilitation program. These seminars will teach you about lung disease and give you coping methods to help you manage your anxiety. How to breathe more effectively is one of the most crucial things you’ll learn throughout pulmonary rehabilitation.
Individual counseling has proven useful in lowering anxiety in people with lung disease. Cognitive-behavioral therapy (CBT) is a typical therapy that uses relaxation methods and breathing exercises to help reduce anxiety symptoms.
Treatment Helps You Live Longer

Some treatments, such as Oxygen Therapy, reduce mortality rates in patients with advanced lung disease. According to the British Medical Research Council Study and the US National Heart, Lung and Blood Institute’s Nocturnal Oxygen Therapy Trial, long-term oxygen therapy improves survival 2-fold or more in hypoxemic patients. In these studies, oxygen was used for 15-19 hours per day, so specialists recommend long-term oxygen therapy followed by a Re-evaluation period with these patients 1-3 months after initiating therapy as some patients may not require long-term oxygen therapy.
DOWNSIDES OF LUNG DISEASE TREATMENT

It’s difficult to find the right treatment that you can afford.
Lung disease is commonly misdiagnosed. Many people with lung disease may not be diagnosed until the disease is advanced. It is often difficult to find the proper treatment for you as lung disease is often misdiagnosed. You may go through a round of oxygen therapy to then find out you have a different form of lung disease that oxygen therapy is not as effective for. There are so many different ways of treating lung disease that it may also be overwhelming for you.
Surgery is an option for some people with some forms of severe lung disease. This is usually reserved for those who aren’t helped significantly enough by medications alone. Surgery options include Lung volume reduction surgery and lung transplant. These surgeries, however, can be costly and might not be the best option. Lung disease treatment can also be expensive. For example, oxygen therapy can add up for those who need it long-term, as you need to purchase oxygen tanks every few weeks or months. At Life Wellness Healthcare, we can help you manage the cost of treatment and find affordable solutions.
TIPS FOR KEEPING YOUR LUNGS HEALTHY AND FUNCTIONING PROPERLY
Know you know the basics of taking care of your lungs, but here are a few more tips to keep them healthy. With these tips, you can help your lungs stay healthy for years.
Avoid Smoking and Second-hand Smoke

One of the best things you can do for your lungs is to avoid smoking. If you smoke, quitting is the best way to improve your lung health. Secondhand smoke is also harmful, so it’s important to avoid being around it as much as possible.
Stay Active and Exercise Regularly

Exercise is good for your overall health, and it’s especially beneficial for your lungs. Regular exercise can help keep your lungs healthy and functioning properly because it strengthens your respiratory muscles.
Stay Hydrated

Drinking plenty of fluids is important for overall health, and it’s especially crucial for lung health. Staying hydrated helps keep mucus thin and makes it easier to expel from the lungs.
Avoid Pollutants and Air Pollution

Pollutants in the air can be harmful to your lungs. It’s important to avoid exposure to air pollution as much as possible. Try to stay indoors when the air quality is poor, and if you have to go outside, try to do so during times of the day when the air quality is better.
Wear A Mask When Necessary

If you’re going to be exposed to pollutants or other harmful substances, it’s important to wear a mask. This will help protect your lungs from the harmful particles in the air.
Eat Foods Rich in Antioxidants

Antioxidants are beneficial for overall health, and they can also help improve lung function. Foods like fruits, vegetables, and whole grains are all excellent sources of antioxidants.
See Your Doctor Regularly for Check-ups

It’s important to see your doctor regularly for checkups, especially if you have a history of lung problems. Your doctor can help monitor your health and ensure that your lungs are functioning properly. Doctors can also help identify potential issues early on and offer treatment options.
Find A Reliable Treatment
As mentioned, finding a reliable treatment is important if you have a history of lung problems. Many options are available, so it’s important to find one that works for you. We recommend our quality OPEP device, which provides a long-term solution for your lung problems.
THE OPEP DEVICE
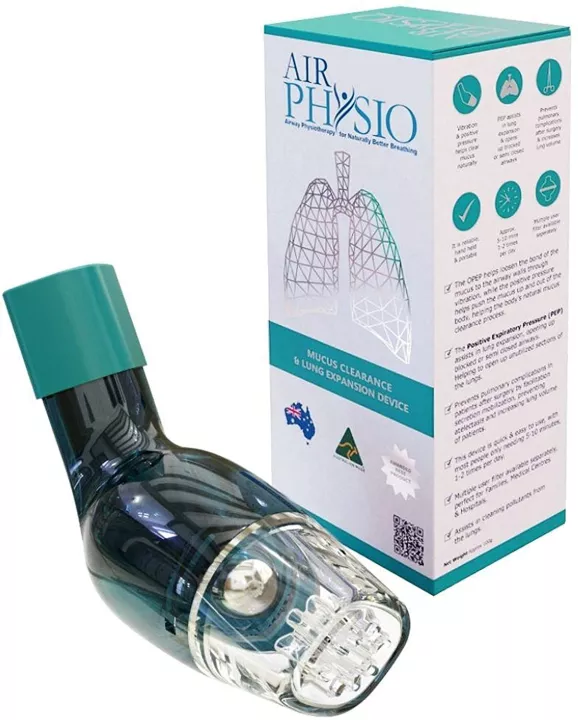
If you have ever had asthma, you know how important it is to have a reliable breathing device. For many people, this means using an inhaler regularly. However, a new device on the market may provide a more efficient way to breathe. The OPEP Device is designed to improve airflow and help people breathe easier. Read on to learn more about this innovative product and how it can help you live a healthier life.
WHAT IS AN OPEP DEVICE?

The OPEP device is a natural way to treat respiratory problems and improve lung function. It is an oral device that helps open the airways, making breathing easier. The device is made of soft, medical-grade poly-carbonate and fits snugly in the mouth. It is easy to use and can be worn for any length of time. If you are an athlete or a heavy smoker with asthma, the OPEP device will improve your everyday breathing performance.
HOW DOES THE OPEP DEVICE WORK?
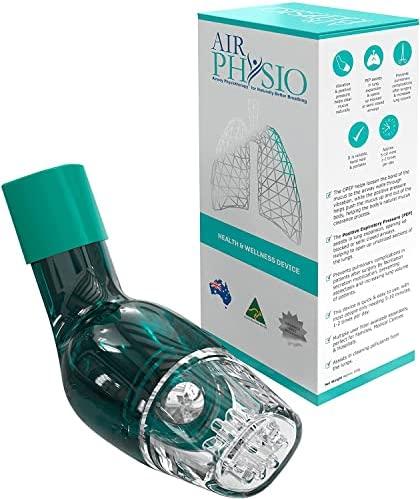
An OPEP device can help with congested airways in two ways: oscillations and positive pressure.
Oscillation: The stainless steel “flutter” ball sits atop the gadget on a cone. The ball travels higher and downward from its resting position as the patient exhales into the OPEP device, creating the Oscillation (OPEP) or vibration.
The vibrations then resonate throughout the patient’s airway, aiding in the mobilization of mucus, phlegm, and irritants.
Positive Pressure: Positive pressure signifies the presence of gases in space or regions. When you exhale through a flutter valve device, positive pressure is created along the airways, keeping them open. Exhaling with resistance opens the airways, allowing more waste products like carbon dioxide and mucus to flow through and escape.
The OPEP gadget opens up the airways while the flutter ball reduces the stickiness of the mucus, allowing more mucus to be ejected during the coughing phase of PEP Therapy.
BENEFITS OF OPEP DEVICE

- The OPEP device is easy-to-use and can be used at any time
- It is made of soft, medical-grade poly-carbonate and fits snugly in the mouth.
- The device helps open the airways, making it easier to breathe.
- An OPEP device can help with congested airways
- An OPEP device is not only affordable but also available for purchase online.
- The OPEP device is a natural way to treat respiratory problems and improve lung function.
HOW EFFECTIVE ARE OPEP DEVICES?
Patients with COPD, Cystic Fibrosis, Bronchiectasis, and Asthma have had success with OPEP devices. Increased mucus clearance and cost-effectiveness are two frequent side effects. They’ve grown in popularity in recent years due to the constant outcomes they’ve produced.
THE FOLLOWING ARE OPEP’S IMPACTS ON VARIOUS DISEASES:
- Bronchiectasis: The researchers used a Patient Evaluation Questionnaire in a 2016 study of 14 individuals with Non-CF Bronchiectasis (PEQ). The patients were asked to rate their difficulties on a scale of 0 to 10, with 0 indicating no trouble and 10 indicating extreme difficulty.
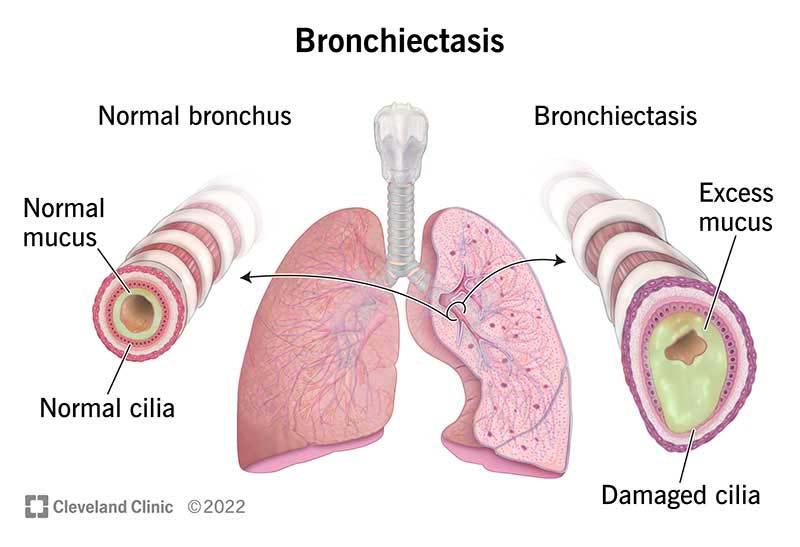
The patients stated that their ability to evacuate mucus improved after three weeks of daily treatment with OPEP devices. Before using OPEP devices, the average reaction was 4.0, but after using them, it was lowered to 2.9. This demonstrates that patients find it simpler and more controllable to discharge mucus after utilizing OPEP devices.
Patients also reported a lessening of the disease’s effect on themselves, in addition to improved mucus discharge.
- COPD: The researchers used a PEQ in a comparative trial of 27 individuals with COPD. The study looked at the effects of OPEP devices for 21 to 28 days. Patients with Bronchiectasis had comparable findings. The patients said they were able to evacuate more mucus. Prior to treatment, the average reaction was 3.9, but it dropped to 2.7 after treatment.
The usage of OPEP devices resulted in more regulated mucus ejection. Furthermore, the usage of OPEP devices has been associated with cost-effectiveness in COPD patients. According to a 2017 study, using OPEP devices saves patients $553 each. This is because there are fewer exacerbations and greater mucus clearance.
HOW TO CLEAN YOUR OPEP DEVICE?
It is critical to clean OPEP devices after each usage since they come into contact with mucus and other biological excretions. This is to avoid additional contamination or infection and the accumulation of moisture in the device. When utilizing OPEP devices, two types of cleaning are recommended: light cleaning and comprehensive cleaning.
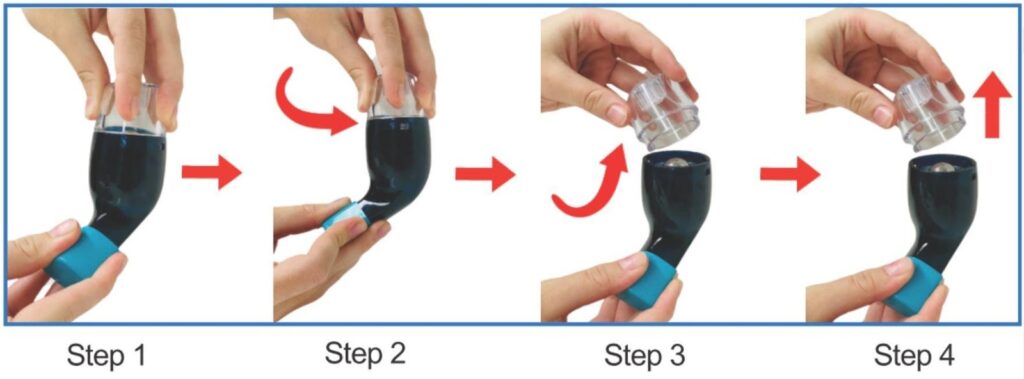
Every time a PEP treatment session is concluded, this cleaning is performed. To do a mild cleaning, just disassemble the OPEP device (follow the instructions in the user’s handbook to prevent breaking anything) and thoroughly rinse all components with tap water. After that, dry well with a clean cloth before reassembling. Ensure that the item is kept in a dry environment away from direct sunlight.
Every two days, it is advised that you clean thoroughly. Disassemble the device and wash it with a mild soap and water solution or a detergent and water solution to ensure a thorough cleaning. After cleaning, rinse well with fresh tap water, pat dry with a towel, and reassemble the set. A dry place, away from direct sunshine, is again used to keep the item safe.
WHERE IS THE OPEP DEVICE MADE?

AirPhysio, an Australian company, creates this device. AirPhysio has over 20 years of experience in the medical industry, focusing on pulmonary rehabilitation devices.
HOW TO USE YOUR AIRPHYSIO OPEP DEVICE?

Simply place the mouthpiece in your mouth and seal your lips around it. Exhale forcefully through the OPEP device to create a vibration in the chest that will help loosen and expel mucus from your lungs. The design of this product also allows you to inhale deeply and slowly after each exhalation to help clear out any residual mucus.
It’s important to keep in mind that OPEP devices should only be used when you are experiencing difficulty expelling mucus. Otherwise, using the device can lead to more congestion. If you’re not sure whether or not you should use an OPEP device, consult with your doctor.
Remember to stop inhaling and exhaling if you feel dizzy or lightheaded. These are signs that you are using the device too forcefully. If you experience any pain while using the OPEP device, stop immediately and consult with your doctor.
WHERE TO BUY YOUR AIRPHYSIO DEVICE?

At Life Wellness Healthcare, we believe that everyone deserves to breathe easily. That’s why we offer the AirPhysio OPEP device at an affordable price. We also offer free shipping on orders over $100. So, if you’re looking for a way to improve your lung health, be sure to check out our selection of AirPhysio products! Shop here.
LIFE WELLNESS HEALTHCARE
Who Are We? 
Life Wellness Healthcare was founded to satisfy the requirements of those who live with respiratory and other diseases every day. We know firsthand what it’s like to live under such conditions—it may be difficult—so we’re dedicated to providing solutions that fulfill the demands of the clients we serve. Our goal is to assist people in regaining their confidence and lifestyle independence.
What Do We Offer?
We offer an OPEP device of the highest quality made with your comfort in mind. Our device is easy to use and helps loosen mucus so you can expel it from your lungs more easily. We also offer a variety of other respiratory devices and solutions and educational resources so you can live life to the fullest despite your respiratory disease. Along with the following
- A Wide Range of AirPhysio Devices
- Free Shipping on All Orders Over $100
- 30-Day Money-Back Guarantee
Are We AirPhysio?

No, we are simply a leading distributor of AirPhysio devices in the United Kingdom. We are committed to providing our customers with access to the highest quality respiratory health products available.
To purchase our spectacular range of AirPhysio devices, visit our website. If you have any questions about our products, contact us today to find out more.
THE COST OF PREVENTATIVE CARE AND HOW TO MAKE IT MORE AFFORDABLE
As you already know, the cost of maintaining your health, never mind your lung health can be costly. So how can you make preventative care more affordable?
There are a few things you can do:
- talk to your doctor about ways to reduce the cost of medication or procedures
- look into health insurance plans that offer lower rates for preventative care
- Invest in a medical savings account (MSA) to help pay for future medical expenses
- Take advantage of tax breaks for preventative care expenses
- Preventative care is important for everyone, but it’s especially
- Invest in a quality OPEP OPEP device today to help improve your lung health and make preventive care more affordable. Our devices are easy to use and have a money-back guarantee, so you have nothing to lose. Visit our website now to learn more. Thanks for reading!
KEEP UP TO DATE WITH LIFE WELLNESS HEALTHCARE – YOUTUBE, FACEBOOK, TWITTER, AND INSTAGRAM

At Life Wellness Healthcare, we pride ourselves on our quality products, but we are also leaders in respiratory health education. Our blog is a vital part of this, providing valuable insights into all aspects of lung health – from tips and advice on keeping your lungs healthy to the latest news and research in the field. Here you will find everything you need to know about lung health, from the basics to more specialist topics.
We understand the importance of respiratory health, and we are committed to providing you with the latest information, resources, and support. Keep up to date with us on our social media channels – YouTube, Facebook, Twitter, and Instagram – and make sure you never miss out on a thing!
We hope you find this information helpful and that it helps you to keep your lungs healthy and functioning at their best. If you have any questions or would like further information, please don’t hesitate to get in touch with us – we’re always happy to help.
Life Wellness Healthcare & Airphysio FAQs

Are these devices safe?
Both the AirPhysio device and our other products are made from high-quality, medical-grade materials and have been designed for safety and comfort. They have been registered with the European CE, United States FDA, Australian TGA, and other international territories.
Do I need a prescription?
No, you do not need a prescription. These devices are classed as Over The Counter (OTC) medical devices.
Can I use these devices if I am pregnant?
There is no evidence to suggest that using these devices is harmful during pregnancy. However, we recommend that you consult your GP or midwife before using them.
How often should I use the devices?
We recommend that you use the devices when you feel you need them. However, for best results, we recommend using them daily.
Can I use the devices if I have asthma?
If you have asthma, we recommend consulting your GP before using the devices.
Can young people use this device?
People of all ages can use the devices. If you are under the age of 18, we recommend that you consult your GP before using the devices.
How long will the effects last?
The effects of using the devices are usually long-lasting. However, we recommend that you use the devices regularly to maintain optimal lung function.
Do I need to clean the devices?
Yes, you should clean the devices on a regular basis, following our recommendations.
If you have any other questions about our products or services, please don’t hesitate to get in touch – we would be happy to help.
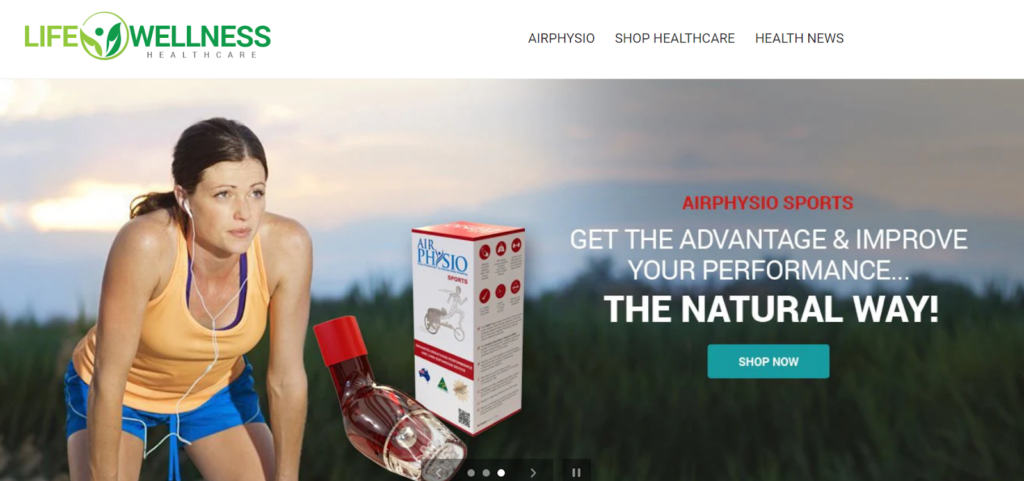
Average Lung AirPhysio
ENJOY BETTER BREATHING - Use this 100% Drug Free Device - AIRPHYSIO
Recent Posts
Sports AirPhysio
IMPROVE YOUR SPORTING PERFORMANCE - Use this 100% Drug Free Device - AIRPHYSIO

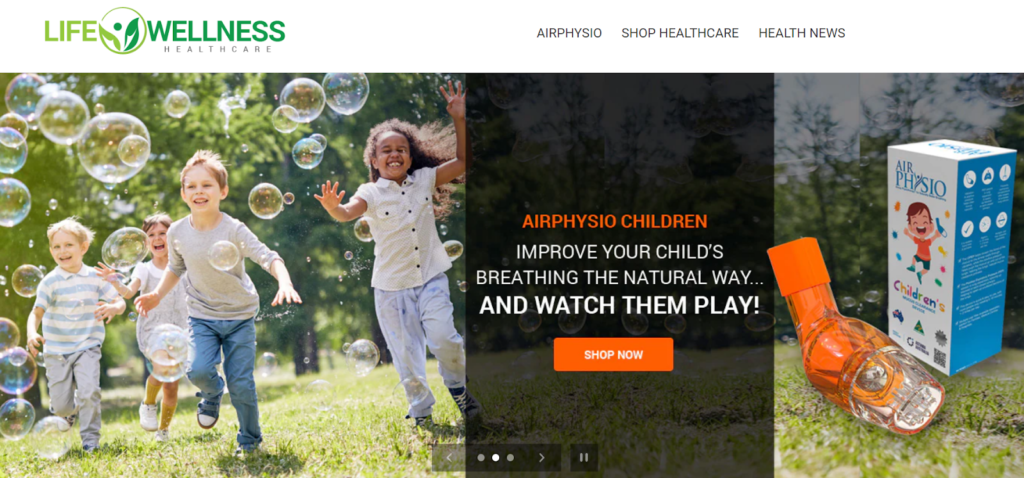
AirPhysio Child
BETTER BREATHING FOR YOUR CHILD - Use this 100% Drug Free Device - AIRPHYSIO

Categories
- asthma (2)
- atelectasis (2)
- bronchiectasis (2)
- copd (3)
- cystic-fibrosis (45)
- featured (10)
- uncategorized (2)


