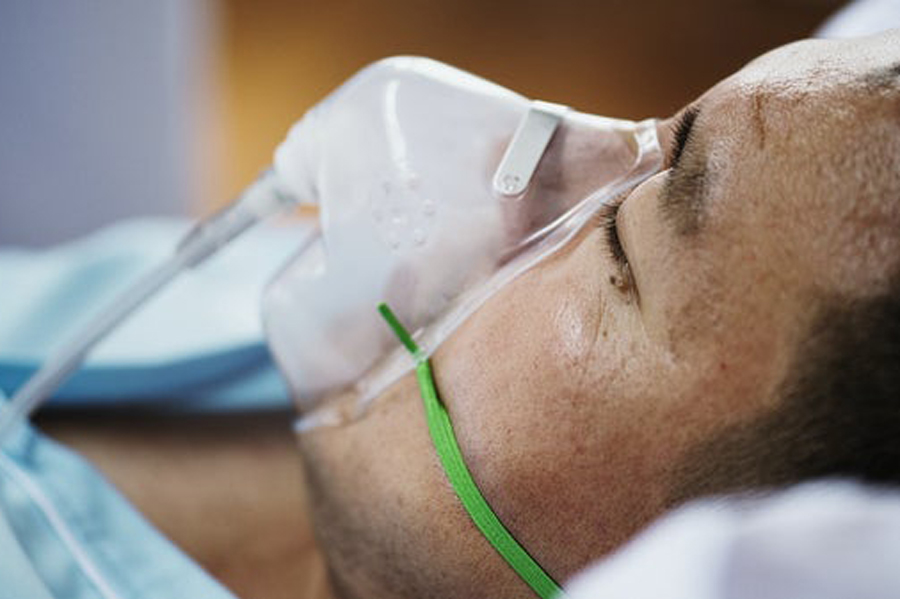
Can COPD Be Reversed? Here’s What You Need to Know
COPD, which is short for Chronic Obstructive Pulmonary Disease, refers to a group of progressive lung disorders that make it difficult to breathe. The condition is the number three cause of death in the US, with more than 15.9 million people diagnosed with the illness.
Experts estimate that millions more may have COPD without even knowing it. The disease has serious long-term health complications and may lead to disability and early death, especially if left untreated.
The most common forms of COPD are chronic bronchitis and emphysema. Bronchitis leads to the inflammation of the bronchial tubes, which causes them to narrow and mucus to build up. Emphysema, on the other hand, slowly destroys the air sacs, which then gets in the way of the outward flow of air.
One of the most frequently asked questions by people with the condition is – Can COPD be reversed? Here’s what you need to know.
WHAT CAUSES COPD
Most of the individuals with COPD are usually over 40 years old, with some form of a smoking past. Smokers generally have a higher risk of COPD. It’s not just cigarette smoke either. Secondhand smoke, pipe smoke, and cigar smoke can all cause the condition. If you already have asthma and you smoke, your risk of COPD is even higher.
Additionally, if you live or work in an environment where you’re constantly exposed to chemical and industrial fumes, air pollution, and dust, all these are potential causes of COPD, which puts you at risk of developing the condition.
Researchers have also found that some people may have a genetic predisposition to developing the condition. An estimated 4 to 5 percent of individuals with COPD are deficient in alpha-1 antitrypsin. This is a protective antitrypsin produced in the liver, which balances the effects of neutrophil-protease enzymes in the lungs.
Some of these enzymes, such as neutrophil elastase, are released by neutrophils when there’s an infection, inflammation, or as a result of smoking. There may also be other genetic factors at play.
HOW TO TELL IF YOU HAVE COPD
In the early stages of the illness, the symptoms can be quite subtle. In most cases, you might even think you have a cold. Early signs of COPD include:
- A mild but persistent cough
- An overwhelming urge to clear your throat frequently, especially when you first get up in the morning
- Unusual shortness of breath, especially after engaging in physical activity
As the condition continues to get worse, the symptoms get harder to ignore. As a result, you may notice:
- A chronic cough that may or may not have mucus
- A general lack of energy and feeling of fatigue
- A high-pitched sound (wheezing) when you exhale
- A need to clear mucus from your lungs every day
- Frequent respiratory infections like colds and flu
- Shortness of breath even with moderate levels of exertion like walking up a flight of stairs
- Tightness in the chest
At advanced stages of COPD, symptoms include:
- Extreme fatigue and lethargy
- Swollen legs, feet, and/or ankles
- Visible weight loss
These symptoms are likely to be aggravated if you smoke cigarettes or any other tobacco products or are frequently exposed to secondhand smoke.
HOW IS COPD DIAGNOSED?
There’s no single test for diagnosing COPD. Your doctor will likely need to do a physical examination and analyze your symptoms before ordering a diagnostic test to rule out other potential respiratory ailments.
Inform the doctor if:
- Someone in your family has COPD
- You have any other respiratory ailments
- You live or work in an environment where you’re exposed to a considerable amount of secondhand smoke or other lung irritants
- You smoke or used to smoke in the past
- You’re currently taking over-the-counter medication
Once your doctor has all the information they need, they’ll then use a stethoscope to listen to your lungs as you breathe in and out. Based on their findings, they may order some tests to get an accurate picture of what could be going on inside your lungs.
The first will likely be spirometry, a non-invasive test used to assess lung function. It involves taking a deep breath and blowing out into a tube that’s connected to the spirometer.
The other test they may order for is a CT scan of the chest or an X-ray. These provide a detailed view of the lungs, heart, and blood vessels.
Finally, they may order an arterial blood gas test, which involves drawing a small blood sample directly from the artery to assess blood oxygen and carbon dioxide levels. This will tell them whether your lungs are working as they should.
Depending on the outcome of these tests, your doctor will be able to tell if you have COPD or an entirely different condition such as heart failure, asthma, or some other kind of restrictive lung disease.
HOW IS COPD TREATED?
Treatment for COPD is designed to manage the symptoms of the disease by slowing down its progression. There’s no cure for COPD. Your healthcare provider will likely bring a pulmonologist and a respiratory therapist on board for your treatment journey.
Here are the various treatment options available for patients with the condition.
Oxygen Therapy
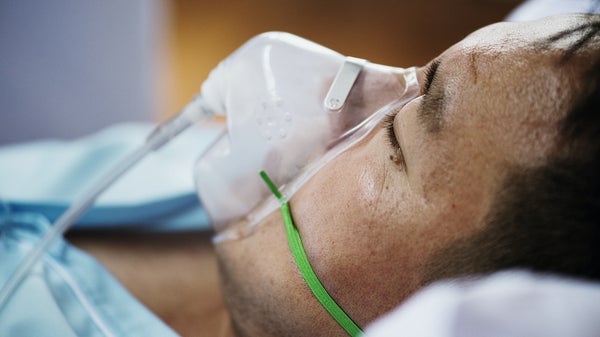
When the lungs are damaged, the shortness of breath you experience results from your body not getting enough oxygen. It’s also why you feel tired and lethargic. Supplemental oxygen administered through a nasal cannula or mask can help you breathe better. There are portable units available that make it easier to get around.
Surgery
In severe cases of the condition, surgery may be the only viable alternative after all other treatments have failed. This is particularly common in severe forms of emphysema. Depending on what your physician prescribes, there are generally four types of surgery available to individuals with severe COPD.
- Bullectomy – This procedure involves the removal of abnormally large, damaged air sacs (bullae) from the lungs
- Lung reduction – This removes damaged lung tissue in the upper portions of the organ
- Lung transplantation – This may be an option in some cases; the patient gets a new set of lungs
- Endobronchial valves (EBV) – This is the least invasive option and involves implanting one-way valves to divert airflow away from the damaged, non-functioning lungs to the healthy ones
Surgery
You can make certain changes to your lifestyle to help alleviate COPD symptoms and provide some relief. These include:
- Avoiding secondhand smoke, chemicals, fumes, dust, and other potential sources of exposure
- Quitting smoking
- Eating healthy for your body to get the nutrients it needs for healing and repair
- Exercising regularly (based on your doctor’s recommendations) to keep your lungs strong

CAN COPD BE REVERSED – THE ROLE OF MEDICATION IN TREATMENT
Currently, no medication can reverse the effects of COPD. However, preliminary clinical trials show promising results in using stem cells to regenerate lung tissue, effectively reversing the damage.
The existing medications for COPD can reduce the symptoms of the disease and flare-ups. While no two people respond to medication the same way, doctors usually use an element of trial and error before they find what works for you. Here are some of your options:
Corticosteroids
These can be administered through inhalers and nebulizers, although they are also available in pill form. They work to reduce inflammation in the airways, which effectively lowers mucus production in the lungs, making it easier to breathe. The most common corticosteroids that doctors prescribe are fluticasone, budesonide, and prednisolone.
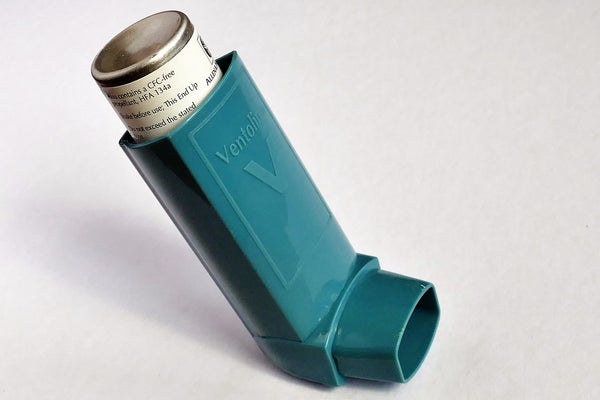
Inhaled Bronchodilatorsticosteroids
These work to relax the tight, restrictive muscles of the airways in the lungs. They are usually administered through an inhaler or a nebulizer. Short-acting bronchodilators are effective for between four and six hours and are typically used as needed. Albuterol, levalbuterol, and ipratropium are the most common bronchodilators.
If, on the other hand, your COPD symptoms are ongoing, your doctor may put you on long-acting medication that you’ll need to take every day. These are usually effective for about 12 hours. The most common ones include aclidinium, arformoterol, formoterol, and indacaterol.
Phosphodiesterase-4 Inhibitors
These are available in pill form and work to reduce inflammation in the airways, as well as relax them to make it easier for patients with COPD to breathe. Phosphodiesterase-4 inhibitors are prescribed for severe cases of COPD with chronic bronchitis.
Roflumilast the most common phosphodiesterase-4 inhibitor your doctor is likely to prescribe and is usually taken alongside a long-acting bronchodilator. If you suffer from depression or have any liver problems, be sure to mention this to your doctor before you start taking this medication.
Methylxanthines
The usual range of first-line treatments like bronchodilators and corticosteroids are not usually effective when used on their own among people with severe COPD. In such instances, your doctor may prescribe theophylline along with them.
This methylxanthine helps relieve shortness of breath and chest tightness by relaxing the muscles in the airways. Keep in mind that it may cause unpleasant side effects like nausea, vomiting, headaches, trouble sleeping, and insomnia in some individuals.
Antibiotics and Antivirals

If you develop a respiratory infection while you have COPD, your doctor will likely prescribe antibiotics and antivirals to treat the condition.
Vaccines
To reduce your risk of other respiratory infections if you already have COPD, it might be a good idea to get your annual flu shot and pneumococcal vaccine. You may also want to get a tetanus booster shot that also includes protection against whooping cough. Make sure you consult with your doctor before you do.
WHAT IS THE OUTLOOK FOR COPD TREATMENTS?
Researchers and doctors continue to work tirelessly to develop new medications that can help improve breathing among individuals living with the condition. So far, several clinical trials are evaluating the effectiveness of biologic drugs designed to target the source of inflammation in the lungs.
A new drug called anti-interleukin 5 (IL-5), for instance, targets inflammation in the eosinophilic airway. Most people who suffer from COPD have a higher-than-usual number of eosinophils, one of the several types of white blood cells that exist.
If approved, IL-5 will dramatically reduce the number of eosinophils present in the blood, which will, in turn, provide relief to those with COPD. However, it’s important to note that there are currently no biologic drugs that have been approved for the treatment of the disease.
DOWN BUT NOT OUT
Can COPD be reversed? Although stem cell therapy shows promising results, there’s currently no way to reverse or completely cure COPD. However, it is possible to reduce the symptoms and slow down the progression of the disease for a better quality of life.
Making changes to your lifestyle like quitting smoking and steering clear of environmental pollutants will also go a long way in reducing the symptoms and slowing the progression of the disease. Talk to your doctor about the treatment options available to help manage your symptoms.
Can asthma go away? The answer to this might surprise you. Check out our blog to learn more.
Average Lung AirPhysio
ENJOY BETTER BREATHING - Use this 100% Drug Free Device - AIRPHYSIO
Recent Posts
Sports AirPhysio
IMPROVE YOUR SPORTING PERFORMANCE - Use this 100% Drug Free Device - AIRPHYSIO

AirPhysio Child
BETTER BREATHING FOR YOUR CHILD - Use this 100% Drug Free Device - AIRPHYSIO

Categories
- asthma (2)
- atelectasis (2)
- bronchiectasis (2)
- copd (3)
- cystic-fibrosis (45)
- featured (10)
- uncategorized (2)